
Introduction
Many suggestions for improvements to the health care system are centered around the elderly or critically ill, but we often forget about the little ones in our homes. According to data from the National Center for Health Statistics, nearly 16 million children aged 5-17 have missed one or two days of school in 2012 due to illness or injury while another 12.7 million have missed 3-5 days.
School nurses are among those with the most up-close and personal perspective on the wellbeing of young students. Not only can they assist with their day-to-day physical health problems, but they can step up and assume a greater leadership role in other areas.
Here are a few examples:
- Counseling Sessions – School nurses are trained to provide mental health service to their students. This includes the ability to refer them to proper mental health resources and channels.
- Health Education – Spearheading campaigns to educate parents, families, and students about ways they can prevent ailments from spreading.
- Wellness – Keeping students healthy begins by fostering a healthy learning environment for all.
- Community Outreach – A healthy schooling environment is much easier when we have community support. School nurses can help in this way by providing a liaison between local health advisory committees and parents.
- Nutrition – One aspect that seems to fall by the wayside for many busy families is the ability to eat healthy food on a consistent basis. Schools have been working tirelessly for many years to provide healthy meal choices for all students.
- Physical Fitness – Students need to get active on a daily basis. By working with school staff and athletics coaches, nurses can help create a program that ensures kids reach these fitness goals.
Common Illnesses
What are the most common student illnesses that are spread in schools? Let’s name a few.
Pink Eye
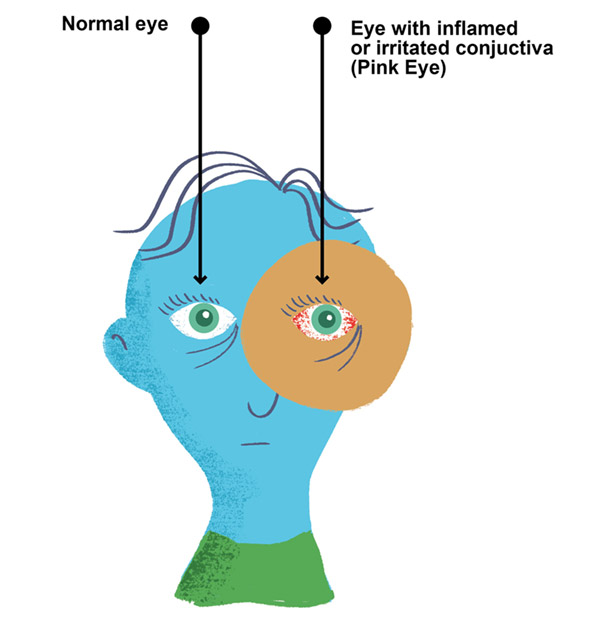
One of the most highly contagious childhood afflictions is “pink eye”—something we’ve all probably dealt with once or twice in life. Conjunctivitis involves the inflammation of the membrane that covers our eyes and eyelids.
There are three types of conjunctivitis, allergic, bacterial, and viral. Here are the symptoms that each of these has in common:
- Excessive tearing
- Burning, itching sensation
- Swelling the eyelid or eyeball
- Thick discharge
- Crust forming on eyelids
- General redness
Types of Pink Eye and Treatment Methods
Taking our concept of conjunctivitis a step further, let’s delve into the various types of pink eye and the methods in which they can be treated.
Allergic Pink Eye
Oftentimes a seasonal variant of pink eye, this type occurs when pollen counts are at their highest. Children who suffer from allergies to animal dander or pollen or those who have asthma are particularly easy targets.
Bacterial Pink Eye
Associated with an earache or other respiratory infection, this is accompanied by a fairly thick discharge leading to only one eye being infected.
Viral Pink Eye
Going hand in hand with a cold or sinus infection, this usually affects both eyes and involves a watery discharge. Thankfully, it can typically be remedied on its own over the course of one to two weeks.
How to Clean Pink Eye
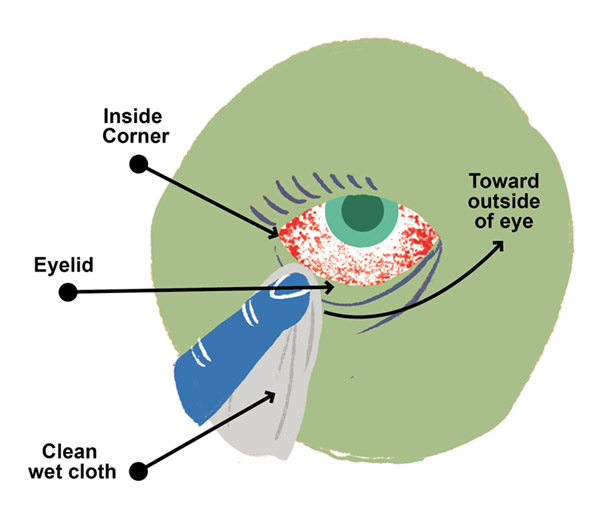
With regular at-home cleaning, a pink eye case should clear up on its own. If it doesn’t get better, take the individual to the doctor to see if anything else is wrong.
If your child exhibits any of these symptoms after having their eyes cleaned, then a visit to the doctor is essential:
- Heavy Redness (more than usual)
- Sensitivity to Light
- Blurred Vision
- Bacterial Pink Not Going Away
While each school or daycare facility will have its own rules regarding students who are infected with pink eye, it’s widely advised that children should stay at home until their eye ceases tearing or producing a discharge. Expect a child to need anywhere from 3-7 days at home for their recovery, with the possibility of needing to show their school a doctor’s note.
How can you prevent pink eye in the first place? It begins with adherence to good hygiene; washing your hands, not touching your face or eyes, and taking daily showers is a simple way to start.
Strep Throat
One of the most common yet painful infections a child can have is strep throat. In elevated terms, this is caused by group A streptococcus bacteria and is extremely contagious. It can be contracted through the mouth by way of coughing, sneezing, or even sharing a glass with someone who might already be sick.
Identifying Strep Throat
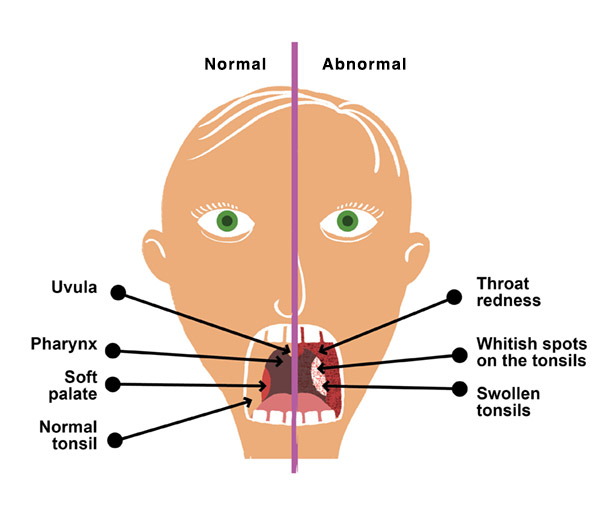
Symptoms of Strep Throat
- Fever of 101 degrees F or greater
- Red or swollen tonsils
- Headache
- Nausea
- Vomiting
- Painful to swallow
- Swollen lymph nodes in the neck
Many of these symptoms probably look like those of a standard sore throat. While it’s true that there are similarities between a normal sore throat and strep throat, it’s important that if the child is in significant discomfort, you take him or her to see a doctor right away. Antibiotics are the necessary cure for strep throat.
It remains contagious until the patient has been treated with antibiotics for 24 hours. Thus, you must keep your child separated from public places during this period.
The bacteria that lead to strep throat live on just about any surface—even on the bristles of a toothbrush.
Parents should talk to their child’s school nurse and figure out the facility’s policy towards strep throat. You mainly need to find out how long your child would be required to miss school after having strep throat.
Head Lice
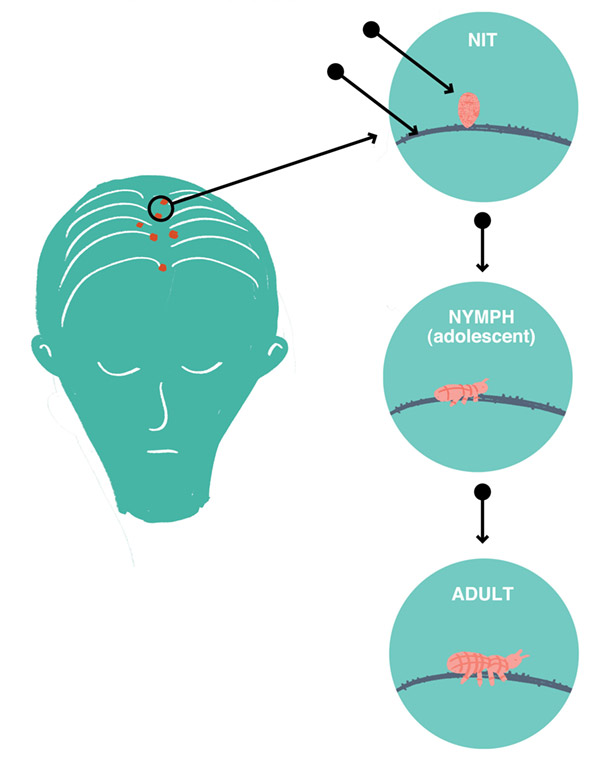
Although head lice won’t hurt you, it can spread rapidly from one child to the next. It quickly forms scalp infestations which survive by feeding on human blood. Its eggs attach to hair follicles near a person’s scalp where adult lice live.
What Questions Should you Ask about Lice?
Q: How did my child get lice?
A: Because lice live on the head and are transferred from head-to-head contact, children can get it simply through sharing a hat, comb, or hairbrush. If you know that your child’s friend or sibling had lice, keep others away from pillows, couches, or beds that the lice-inflicted person came in contact with.
Q: What are the signs of lice?
A: When a child scratches their head and complains of excessive irritability, or is having difficulty getting comfortable.
Q: How do I find lice on my child?
A: You can use a magnifying glass in bright lighting to inspect your child’s hair. Be sure to check at the root level.
Q: How do I get rid of my child’s lice?
A: Experts recommend that you utilize lice medication before trying a shampoo remedy. There are also some home remedies you can try using olive oil—this slows down lice. Be sure to inspect the strands of your child’s hair near the root level.
Q: How do I get rid of lice from inside my home?
A: It’s not just your child that needs to be cleaned of lice, you must also scrub your home.
- Wash all fabrics that your child has contacted in the past 48 hours in hot water; dry using high heat.
- Vacuum upholstery everyday to completely get rid of the lice. This includes furniture that’s covered in fabric.
- Wash hair care products in hot, soapy water.
- Non-washable items in plastic bags for two weeks.
Visual Guide for Removing Lice
Supplies You’ll Need

How To Find Lice
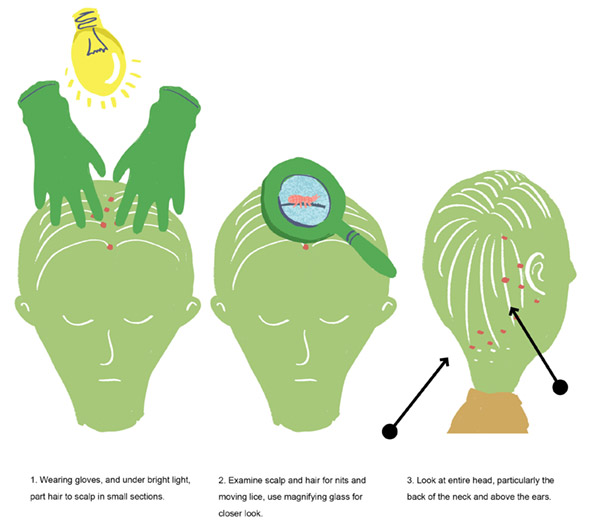
How To Remove Lice
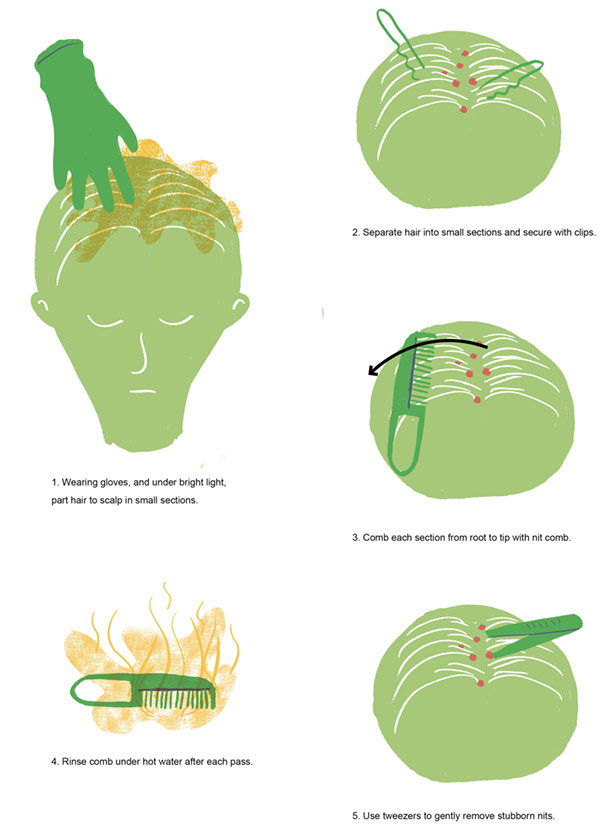
Chickenpox
One of the most common, yet contagious illnesses around is the chickenpox virus. Although it’s usually over in one week to ten days, it may have been contracted by the child up to three weeks earlier since symptoms take time to show up. What are those symptoms? Well, thankfully chickenpox is fairly recognizable to most of us. We recognize it by its patented red rash that appears all over the affected person’s body, combined with their constant need to scratch it. The red bumps which pop up over the course of several days then form blisters which are filled with fluid.
MRSA (left) vs Chickenpox (right)
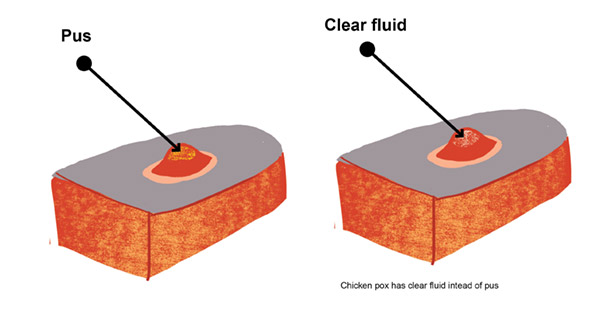
Timeline of Chickenpox
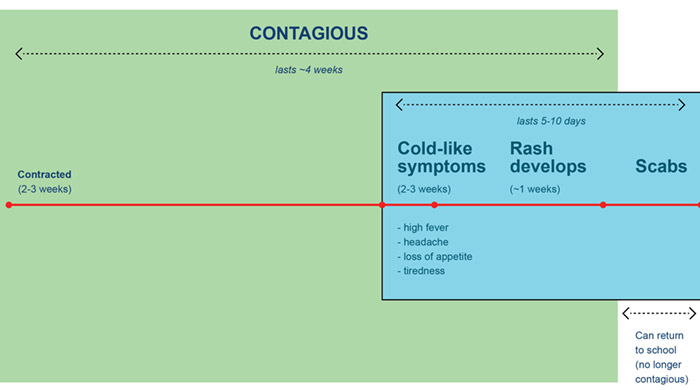
Children with chickenpox remain contagious until their blisters have turned to scabs. Once this occurs, it’s typically fine for them to return to school. To be sure, you should consult your school’s nurse.
If your child might’ve been exposed to the virus, keep them away from individuals who have weakened immune systems. They are obviously more susceptible to catching it than others.
The best way to prevent your child from getting chickenpox is to take the initiative and give them a vaccine. If a family chooses not to take the vaccine option, they must know that the virus can easily be transferred through sneezing or coughing. It’s also possible to get chickenpox from a child who hasn’t yet developed a rash.
Once a child has chickenpox, the only remedy is to allow it to go through its paces. That being said, there are ways you can mitigate the pain of the person who has it. One method is to use a non-aspirin pain reliever in order to lower a child’s temperature, accompanied by calamine lotions to reduce itching.
MRSA: Methicillin-Resistant Staphylococcus Aureu
Similar in appearance to chickenpox, a child could have MRSA. These are also pus-filled spots, but they don’t necessarily mean your child has a fever, or chickenpox.
MRSA is a somewhat recent phenomenon which has formed in response to the use of antibiotics to treat infections. While it used to be acquired strictly in a hospital setting, MRSA has now reached the point of being spread outside of a healthcare setting, into the community.
How does MRSA enter the body? Through a puncture in the skin—like a cut or scrape. The area around the puncture becomes very red and inflamed, and oftentimes will fill up with pus. MRSA skin infections can occur anywhere on a person’s body, but the most common places are the buttocks, groin, legs, and back of the neck. Even if your child doesn’t have a fever right now, it’s important that you begin monitoring the progress of the illness; let the school nurse know as well.
MRSA is serious business and requires a visit to a doctor who can help the person drain the infected area.
The best way to protect yourself against MRSA is simply to use proper handwashing. Take regular baths and focus on keeping the skin clean. It’s also very important to wash your face multiple times a day to alleviate the pores.
Be sure to clean all bedding and clothing that comes into contact with the infected areas. This will prevent the infection from spreading.
Common Cold Versus the Flu
Distinguishing a common cold from a more serious sickness, the flu, is not intuitive. They both manifest themselves in aches and pains, sore throats, nasal congestion, and excessive coughing or wheezing. What do the two have exactly in common and what components may be different? Let’s have a look.

There are two factors that are clear: Body aches are much more intense with the flu; fever is a primary component of flu sufferers, and that fever is more sustained. Additionally, a cold can be dealt with in under a week, while flu symptoms might be felt for two weeks or longer.
Prevention begins and ends with good hygiene. Doing things like washing your hands regularly, cleaning the surfaces throughout your home, and avoiding touching your face with dirty hands are all crucial to flu avoidance.
Just as there is a vaccine for chickenpox, there’s a vaccine that individuals can take for the flu. In fact, it’s advised you go and receive a flu vaccine each year during autumn.
If you do catch the flu or even a cold, be sure to drink plenty of fluids every day. If the flu starts to get worse, talk to your doctor about antiviral medication options.
Basic Personal Hygiene Musts
Personal hygiene cannot be taken lightly. Indulging in good hygienic practices will prevent the spreading of germs throughout your home and onto your possessions.
Handwashing
There’s a basic 5-step procedure for effective hand washing as laid out by the Center for Disease Control (CDC). It includes the following:
How to Wash Your Hands
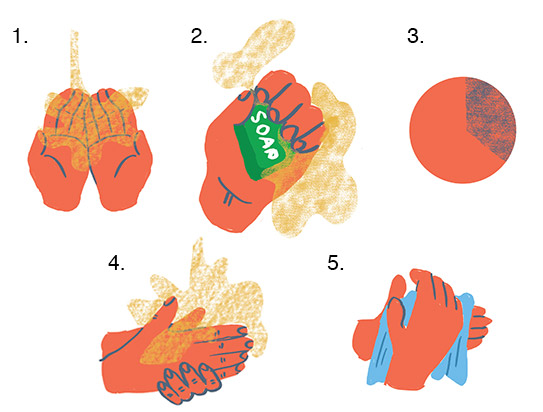
What is the right way to wash your hands?
The step-by-step process goes like this:
- Wet your hands with water and apply soap
- Lather your hands in the soap, be sure to get both the front and back of your hands
- Scrub for at least 20 seconds
- Rinse your hands under clean running water
- Dry your hands with a clean towel
Whether you’re at home or in a workplace, regular handwashing is a must. What constitutes regular hand washing?
As outlined by the CDC, this includes washing your hands at all stages of preparing food (before, during and after). It’s also necessary to do before eating food, before caring for someone who is ill, and before tending to an open wound.
You should also wash your hands after using the toilet, blowing your nose, coughing and sneezing. Do it after touching garbage, feeding your pet, or cleaning up after your pet. And for those with babies at home, always wash after changing a diaper.
Here’s a video showing the proper way to wash your hands, and an explanation of the science behind it.
What do I do if I don’t have soap or running water?
Although it’s not as ideal as washing your hands with soap and running water, you can clean them using an alcohol-based hand sanitizer—it should contain at least 60% alcohol. This will reduce the amount of germs on your hands significantly BUT it won’t rid you of all types of germs. It also won’t be as effective if your hands are particularly dirty or greasy, and it won’t remove all types of chemicals.
Be careful when using hand sanitizer, especially with children. Swallowing an alcohol-based substance like this will potentially cause alcohol poisoning.
How do I use hand sanitizers?
You apply the sanitizing gel to your hand, rub them together, then rub the gel over all surfaces of your hands and allow them to dry.
For a better explanation, read these recommendations, or visit the CDC’s section on handwashing. To ask questions directly, contact CDC-info or call them at 1-800-CDC-INFO.
Never forget to get clean after using the restroom. Germs are all over your restroom, even if you work hard to maintain its cleanliness. It’s important for you to keep yourself clean after every visit, in addition to cleaning your sink faucet and toilet area on a regular basis.
Cover Your Mouth
It should be common sense, but it never hurts to remind individuals that covering their mouth is very important when sneezing or coughing.
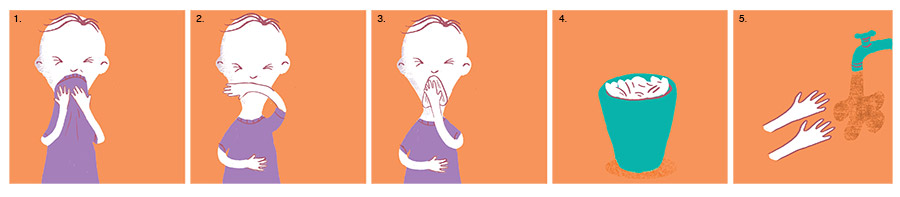
- Cover your nose and mouth completely. Cough/sneeze into your shirt.
- Use your elbow or arm if you need.
- Use tissues when you sneeze or cough.
- Immediately dispose of the tissue.
- Wash your hands afterward.
By simply covering your mouth, you’ll be making huge strides in cutting down the transference of colds and flus.
Children’s Health
In an effort to maintain positive health, we must eat right and properly exercise. Instilling these behaviors within our children from an early age will likely lead them to a healthier adulthood.
Exercise
Regular exercise for children and adolescents is essential for preventing a serious weight gain and preventing Type 2 diabetes. The National Institute of Health recommends children workout for an hour each day. What kind of workout should they do? The CDC outlines several different physical activities children can perform in just 60 minutes each day.
Components of effective exercise include endurance, flexibility, and strength. Endurance is important for a strong cardiovascular system, and results from aerobic exercise. The beauty of cardio workouts is that they can be performed by the whole family. Oftentimes, families working out together can be a great bonding experience as well as being important for improved health.
Children can develop strength from an early age when they engage in regular activities—this includes moving about their local playground, climbing the monkey bars, or shooting hoops at the basketball court.
While it’s true that any physical activity is better than none, there are specific doses of workouts that are highly beneficial. Here are exercises that promote children’s growth and development:
Aerobic
- Running, Biking, Tennis, Basketball.
- Moderate Level – At regular levels, a child can burn between 3 and 7 calories each minute.
- Vigorous Level – When children engage in more rigorous exercise levels, they are likely to burn nearly 10 calories per minute.
Strengthening of Bones
- Running, Jumping Rope, Tennis, Gymnastics.
- One benefit of exercise that often goes unrecognized is the strengthening of a child’s bones. While it’s most crucial to have strong bones later in life, there’s no time like youth to begin promoting bone growth.
Strengthening of Muscles
- Sit-ups or Push-ups, Rock Climbing (indoor or outdoor), Running.
- Increasing muscular strength and tone is another great activity for kids to do from an early age.
What is my maximum heart rate?
Here’s how it plays out for children:
Exercise and Your Heart Rate
| Age | Maximum age-related heart rate (MHR) | Moderate-intensity heartbeats per minute (MBPM) | Vigorous-intensity heartbeats per minute (VBPM) |
|---|---|---|---|
| 5 | 215 | 108 – 151 | 151 – 183 |
| 6 | 214 | 107 – 150 | 150 – 182 |
| 7 | 213 | 107 – 149 | 149 – 181 |
| 8 | 212 | 106 – 148 | 148 – 180 |
| 9 | 211 | 106 – 148 | 148 – 179 |
| 10 | 210 | 105 – 147 | 147 – 179 |
| 11 | 209 | 105 – 146 | 146 – 178 |
| 12 | 208 | 104 – 146 | 146 – 177 |
| 13 | 207 | 104 – 145 | 145 – 176 |
| 14 | 206 | 103 – 144 | 144 – 175 |
| 15 | 205 | 103 – 144 | 144 – 174 |
| 16 | 204 | 102 – 143 | 143 – 173 |
| 17 | 203 | 102 – 142 | 142 – 173 |
| 18 | 202 | 101 – 141 | 141 – 172 |
- MHR – Maximum age-related heart rate: 220 (minus) Age
- MBPM Range: (MHR X 0.50) to (MHR X 0.70)
- VBPM Range: (MHR X 0.70) to (MHR X 0.85)
Nutrition
Exercise is just a small part of a child’s health; another major part is good nutrition. There are many nutritional needs for childhood and beyond, and it’s never too early to start educating kids about achieving proper nourishment. Lessons in portion control, what foods to eat, and making generally healthy decisions can be made at an early age.
Many individuals grew up knowing the food pyramid inside and out. Now, things have changed a little bit, as the food pyramid has been replaced by the MyPlate Food Guide.
Shaped like a plate, this new guide groups four types of foods on it (fruits, veggies, grains, proteins), with a cup of dairy on the side.
The USDA currently recommends people eat more fruits and vegetables than grains, proteins, and dairy products. But does being healthy mean you have to follow these guidelines 100% of the way? Absolutely not. The key is that you’re mindful of the nutritional value in your food and you make purchasing decisions accordingly.
School Lunches
As far as school lunches are concerned, they will largely be governed by the MyPlate criteria, and will have to meet nutritional standards according to the Healthy, Hunger-Free Kids Act 2010.
Here’s a look at what happens when school offer students more vegetable options:
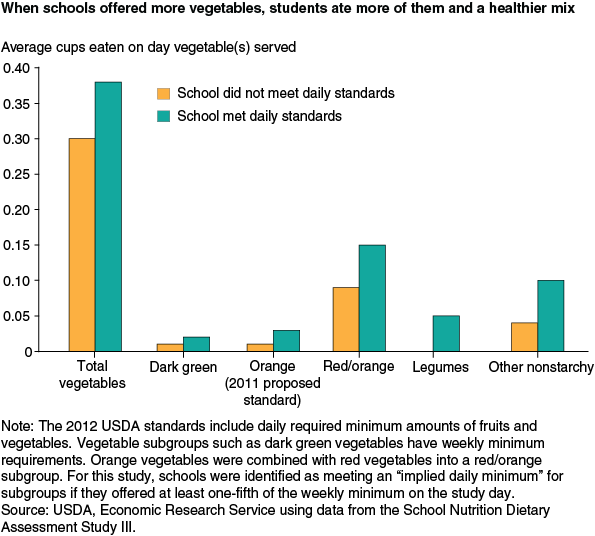
Source: United States Department of Agriculture, Economic Research Service
Here are some simple tips for improved student health, as is being followed by the school lunches program:
- Less salt
- More whole grains
- More fruits
- More vegetables
- More water
Of course, there are also portion sizes to keep in mind depending on a child’s age.
It’s always recommended that parents help their children pack a lunch. This ensures a child will get foods they actually like, and it allows you (the parent) to set their portions accordingly. For example, if a high schooler is playing team sports then they will likely need more calories than a regular kid.
Keep Track of Nutritional Goals
Maintaining a log or journal of your nutritional progress is important for two big reasons.
- Reminding you to adhere to your nutritional goals.
- Showing you the progress you’ve made.
Kids need to see how their actions are playing out, and a journal is the perfect way to show them.
Here are a few resources you may consult to help you reach your health goals:
Awesome Eats – a fun app that teaches children healthy eating through playing games.
MapMyRun – an app that allows users to track their workout and discover fun running routes posted by other users.
Eat-and-Move-O-Matic – advising students about the foods they eat in relation to the energy it provides them. It also describes the physical activities they must do to work off the calories they gain.
FigureFacts Teens – A simple way for teenagers to track their daily food intake in reference to the food pyramid.
Food Allergies in School
Since 1997, an increased number of children have reported suffering from a food-related allergy. While some allergic reactions are minor, others can be life-threatening.
From 1997 through 2011, there appears to be a rise in reported allergic conditions in the United States:
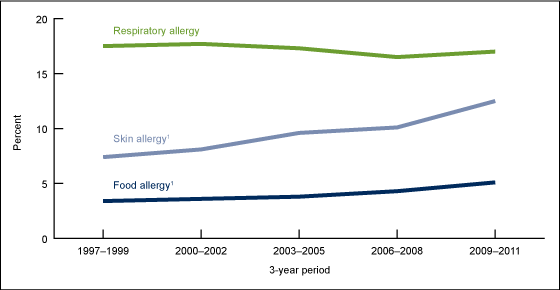
Source: Centers for Disease Control and Prevention
Precautionary Measures
As with many of the afflictions we’ve discussed, the key lies in taking certain preventative measures. A safe learning environment is essential for a food-allergic child.
Schools need to discourage food sharing, disinfect spaces throughout the classroom, be sure to address the allergies of specific students, and have parents call ahead when baking goods for the class.
What should parents do for children with food allergies?
Be sure to provide school nurses with their child’s allergy information, and if serious, have them wear a medical bracelet to school. Disclose the important health information to school officials and administrators.
Food allergies aren’t a one-size-fits-all problem, and each child has their own issues to overcome. In order to best understand what’s going on, adults need to listen for a child’s verbal description about their reaction. Communication is the first step in seeking help.
Anaphylaxis
One of the extreme consequences of allergies is the potential for a person to enter anaphylaxis. This can result in dangerously poor breathing and blood circulation.
According to the Section 504 Plan, when a child’s condition may result in serious or life-threatening reactions, this can be defined as a disability. The plan requires parents and healthcare professionals to setup a written plan of action in case a child is exposed to the harmful allergen.
Concussions
There’s been about a 57% increase in concussions and Traumatic Brain Injuries among student athletes over the past several years. While the likely reason here is that concussions are more widely known today than in prior decades, there still remains a need to understand the risk factors and leading causes of injuries.
Traumatic Brain Injuries are mainly caused by the following:
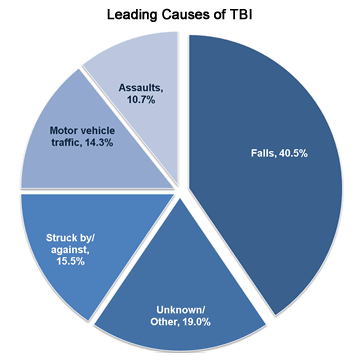
Source: Centers for Disease Control and Prevention
Parents need to identify symptoms of Traumatic Brain Injuries (TBI) when their children are engaged in contact sports.
Recognition and education are paramount, because although proper equipment, sport technique, and adherence to rules of the sport may decrease the incidence or severity of concussions, nothing has been shown to prevent them. – The Council on Sports Medicine and Fitness
Here are the general symptoms to look out for:
-
- Dizziness
- Problems Balancing
Excessive Fatigue
- Nausea
- Confusion
- Slurred Speech
If, on the other hand, you’re experiencing the following symptoms, seek an emergency evaluation immediately:
- Seizures
- Going unconscious
- Repeated Vomiting
- Harsh Headache
- Uncontrollable drowsiness
- Not recognizing familiar people or locations
- Young children refusing to eat
If you’ve been concussed, you may complete this form by way of the American Academy of Pediatrics:
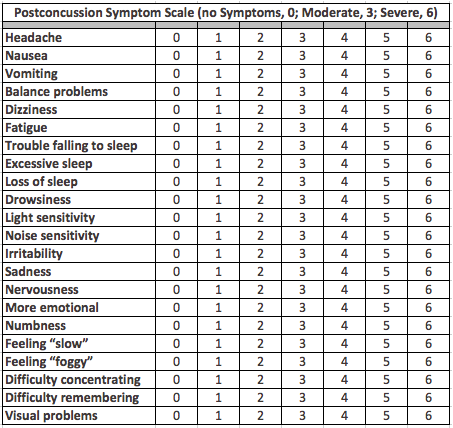
Source: American Academy of Pediatrics
The lesson every parent should take away is not to rush the process. Allow your child to recover before forcing them back into the learning environment, and communicate with their teachers to make sure everyone is on the same page.
Additional Resources
Kids Health & Wellness
- Kids Health Nutrition and Fitness Center
- CDC BAM! Body and Mind Connection
- National Institutes of Health Child Nutrition Resources
- Academy of Nutrition and Dietetics Kids Eat Right
- USDA Child Nutrition Resources
Fitness & Exercise
- PEERtrainer Physical Fitness Resources for Kids
- President’s Council on Fitness, Sports and Nutrition
- American Academy of Pediatrics Fitness
Parenting & Early Learning
- PBS Parents Food & Fitness
- HealthyChildren.org Healthy Active Living for Families
- Parent’s Guide to Healthy Sleep
Other Illnesses to Look Out For
- Enterovirus D68
- Pertussis (Whooping Cough)
- Ringworm
- Severe Acute Respiratory Syndrome (SARS)
- Respiratory Syncytial Virus Infection (RSV)
